How Do You Know if a Pituitary Tumor Is Secreting or Non Secreting?
Pituitary Adenoma
What You lot Need to Know
- Pituitary adenomas are benign tumors of the pituitary gland. Almost are located in the inductive lobe (front portion) of the gland.
- About 1 in 10 people will develop a pituitary adenoma in their lifetime.
- Some pituitary adenomas secrete i or more hormones in backlog. Fifty-fifty when they are small in size, these endocrine-active pituitary tumors can cause hormonal imbalances that impact torso functions.
- People can develop pituitary adenomas at whatsoever historic period.
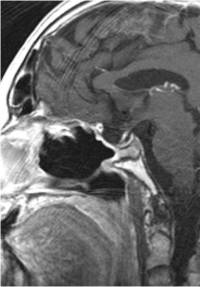
Pituitary Adenoma Symptoms
The symptoms of pituitary adenoma may include:
-
Headaches
-
Vision problems
-
Weight gain
-
Easy bleeding/bruising
-
Modify in bone structure, peculiarly in the face and hands
-
Menstrual irregularities
-
Lactation
-
Erectile dysfunction
-
Heat intolerance

Types of Pituitary Adenomas
Pituitary adenomas are classified by their size and whether or not they secrete hormones.
Endocrine-Agile Pituitary Tumors
Most l percent of adenomas produce excessive amounts of one or more than particular hormones. These endocrine-active tumors are likewise known as secreting or operation tumors. Excessive hormone secretion may cause:
-
Cushing'southward affliction: Due to excessive corticosteroids in the body, Cushing's syndrome can cause a number of symptoms, including:
-
Upper trunk obesity
-
Circular face
-
Increased fat around necK or a fatty hump between the shoulders
-
Thinning artillery and legs
-
Fragile and thin skin
-
Stretch marks on abdomen, thighs, buttocks, arms, and breasts
-
Bone and muscle weakness
-
Severe fatigue
-
Loftier blood pressure
-
Loftier blood sugar
-
Irritability and anxiety
-
Excess facial and body hair growth in women
-
Irregular or stopped menstrual cycles in women
-
Reduced sex drive and fertility in men
-

-
Acromegaly: Excessive growth results in the enlargement of the extremities, face and soft tissues. Acromegaly may be associated with hypertension, diabetes mellitus and cardiovascular disease. Patients with acromegaly accept decreased life expectancy.
-
Galactorrhea: This condition is characterized by abnormal milk product from the mammary glands.
-
Hyperprolactinemia
-
Reproductive problems, such every bit infertility

Prolactinoma is a type of pituitary tumor that overproduces prolactin. The prolactin hormone stimulates milk production from the breasts. Prolactin-secreting pituitary adenomas are the most common type of pituitary tumor, bookkeeping for approximately xxx percent of all pituitary tumors.
Endocrine-Inactive Pituitary Tumors
Endocrine-inactive pituitary tumors do not produce extra hormones. They are also called nonfunctioning or nonsecreting pituitary tumors.

Microadenoma and Macroadenoma
Microadenomas are pituitary adenomas that mensurate less than x mm in diameter (most three quarters of an inch). A pituitary adenoma greater than or equal to ten mm in diameter is called a macroadenoma.
Pituitary Adenoma Diagnosis
Your medico may apply blood tests, urine tests and imaging to diagnose a pituitary adenoma. Blood and urine tests tin can detect abnormal levels of hormones such equally plasma prolactin (PRL), growth hormone (GH), insulin-similar growth factor-1 (IGF-1), gratis thyroxine, cortisol, and testosterone. Abnormal amounts of certain hormones may signal a specific pituitary-related syndrome.
Your physician may also use enhanced, high-resolution MRI technology to place unique characteristics of a pituitary adenoma.
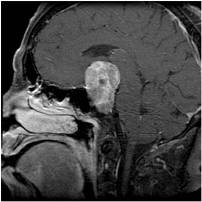
Pituitary Adenoma Handling
The near effective treatments for adenomas are coordinated by a multidisciplinary team that includes a neurosurgeon, otolaryngologist and/or an endocrinologist (hormone disorder specialist). Handling may include a combination of observation, medication (including hormone therapy), radiation therapy and surgery.
Observation
Observation involves seeing a neurosurgeon or endocrinologist who tin prescribe a regular schedule of imaging tests to cheque the status of the tumor. If the pituitary tumor grows or if symptoms worsen, you may need to pursue further handling.
Medication
Medication (drug therapy) can exist very effective in treating some hormone-producing pituitary tumors. It may be used to:
-
End a tumor from producing excess hormones.
-
Shrink the tumor to stop it from pressing on the pituitary gland or other parts of the nervous organisation.
-
Care for a pituitary tumor or control hormones afterward surgery or radiation therapy.
-
Substitute missing hormones if a pituitary tumor has decreased the body'southward power to produce the necessary hormones or if hormone production is too low later on surgery (too known as hormone replacement therapy).

Radiation Therapy
Radiation therapy for pituitary tumors includes external beam radiation therapy and stereotactic radiosurgery. It tin take several months for these treatments to improve symptoms and weather condition related to pituitary adenoma.
Radiations treatment might be advisable for pituitary adenomas that:
-
Are located in areas of the brain where surgery is likewise risky.
-
Cannot be completely removed during surgery.
-
Grow rapidly.
-
Do no shrink with medication.
-
Recur after surgery.
Sometimes radiation therapy tin can crusade the pituitary gland to stop working, even years after treatment. In that case, individuals may need to take hormone supplements.

Surgery
Surgery to remove a pituitary adenoma may rarely require a craniotomy, but more than typically involves a minimally invasive process called an endonasal endoscopic surgery where the surgeon removes the tumor through the nose. It is important to piece of work with a knowledgeable team with a lot of feel in pituitary tumor surgery.
priceupoudiles1941.blogspot.com
Source: https://www.hopkinsmedicine.org/health/conditions-and-diseases/pituitary-adenoma
0 Response to "How Do You Know if a Pituitary Tumor Is Secreting or Non Secreting?"
Postar um comentário